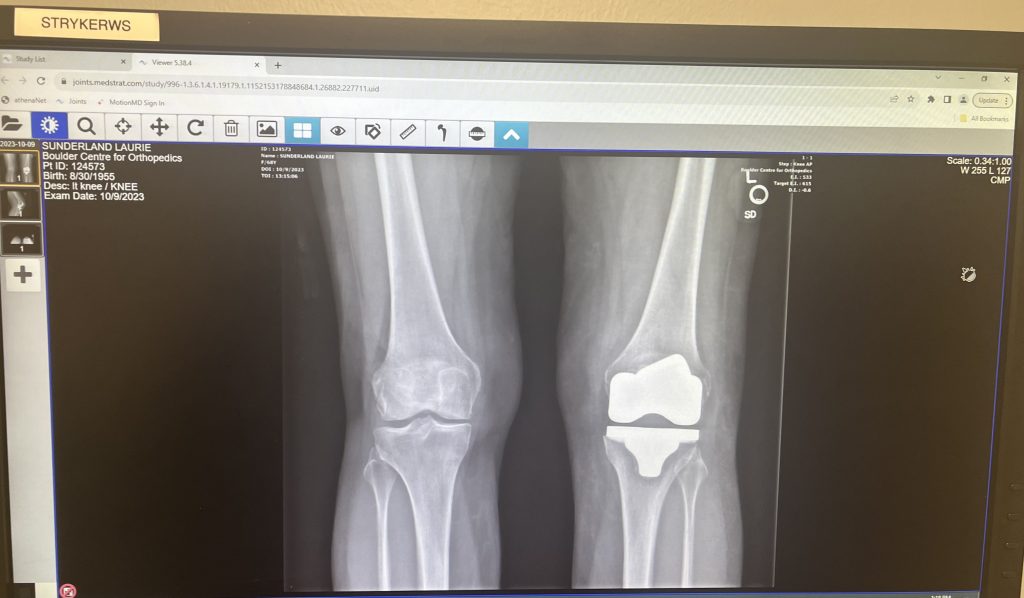
Rhoda’s first portrait (she’s the one that looks a little brighter and shinier than the other one…)
Three and a half weeks ago, I was resting comfortably in the pre-op bed under a heated blanket with my sisters and my daughter seated across the room from me. I remember commenting on how “spa-like” the experience was given the heated blanket. The nurse told me to let her know when the blanket loses its heat and she’d bring me another one, then added that the “spa-like” feeling would be short term. Unlike a spa, I had an IV in my arm and instead of the gentle sounds of nature being piped into the background, I heard doctors being paged. And I was afraid. Afraid because I knew what to expect and the warnings of “it will be painful and the recovery is long and difficult,” were hard to dismiss. (The “warning,” by the way, came directly from my doctor). My left leg was marked with an “X” to indicate it was the knee that was getting “replaced” and below the “X” was my doctor’s signature. Every one who entered the room first asked my name, my birthday and which knee was to be operated on before introducing themselves. I know it was protocol but it became almost comical. I couldn’t help but think about what my 4 year-old granddaughter had asked me a few days before my surgery.
“What if they saw the wrong knee off?”
I told her they check and double check to make sure it’s the right knee before they do any “sawing.”
My doctor had come in briefly and went over the timeline with me, answered my questions and said he’d return when it was surgery time. He wasn’t wearing the usual blue scrubs I was expecting, but instead, had on biking shorts and a tee shirt that looked like it had seen better days. His hair was smashed and misshapen on one side, I’m guessing from the bike helmet. I asked him, jokingly, if he had ridden his bike over and he said he had, but only from a nearby surgery center. Given that this is Boulder where the athleticism is constantly surprising me, that other hospital could have been in Denver.
And now here I sit, 3 1/2 weeks later, on my couch, with my legs not stretched out, not in a massaging ice cuff, but rather, in an 80 degree angle with my feet on the floor. It won’t last very long because it’s still uncomfortable, but for now, I’m sitting like most of the world sits and am feeling pretty proud of the position.
I never knew about knee flexion degrees or angles until a few days after surgery when a physical therapist came to my house and got out her measuring device — a device I would become very familiar with. The oversized protractor, that took me back to my elementary school days and trying to remember which math device was the protractor and which was the compass, now indicates to me that discomfort is coming. When I realized the angle was going to be measured every PT visit, I became competitive (with myself) and would push to get my knee to bend just a tiny bit more than I thought possible. I’ve been told I will probably never have the extension I used to, which would be bringing my heel to touch my backside as in a quad stretch exercise, but I’ll be close. It’s hard to hear things I’ll possibly never be able to do again and I hadn’t given it a thought until the first physical therapist I worked with mentioned that 50% of knee replacement patients can no longer kneel. Really? What if I was Catholic? I’m not, but what if?? What about yoga poses that begin in a kneeling position? She also told me there would be a handful of sports I’d need to give up — basketball, soccer, pickle ball and running for sport. I’m good with that given that none of them are sports I participate in, and as far as the pickle ball goes, I will now have a valid excuse for turning down the many invites I’ve gotten. And one more — skiing moguls. Unless I want to come back in because my replacement has worn out, I’ve been told to stay away from the bumps on the mountains when skiing. I don’t care about any of those things but when you’re told you should never do something again, I’m suddenly interested in women’s soccer leagues and moguls and the Boulder Marathon that was this past weekend. Of course these are activities I never would have taken part in before, but hearing that they are no longer an option if I want to maintain a healthy joint makes me feel like I’m missing out. Even the kneeling, that I may no longer be able to do, is now suddenly appealing to me. There is weight in the word “never.”
My emotions the past three weeks have run the gamut. I’ve been thrilled with my success, discouraged that I’m not further in my recovery, proud that according to the PT’s I’m so far ahead of the game that “if it was a race, you’d be on the other side of the finish line while others are still tying their shoes,” yet discouraged because it still hurts. I’m trying to be patient. I’m trying to give the pain free moments the same amount of time as the ones with pain. I’m trying.
Last week, I went to my first PT session away from my home and I drove. Small victories. Before starting any exercises, my physical therapist had me lay on the table and began removing the steri-strips that had been placed over the incision that was joined with glue. Although it had been three weeks, it still felt like the small line of steri-strips were what was holding both sides of the incision together. I questioned removing them so soon. Ingrid, my therapist, reassured me that the “cement had hardened” and the strips were no longer needed. I couldn’t see what she was doing but still felt uncomfortable with what she was doing.
“I think it’s going to bleed,” I said. As soon as the words left my mouth, I knew how ridiculous they sounded. I thought about my 4 year-old granddaughter who walked into my house a few days earlier barefoot, because she likes shoes but hates wearing them, and noticed she had a bloody big toe. I asked her what happened and did she need a bandaid? Did it hurt? Was she OK? She calmly glanced down to her her toe and said,
“Oh this? Yea. It’s fine.”
She’s 4. Be like Muna, I thought to myself while I braced myself on the table.
Ingrid reassured me that it would not bleed then gave me a towel to put over my face to give me further separation from what she was doing. When she finished, she reassured me that no tourniquets were needed (a sense of humor is a bonus for physical therapists), and she was finished and although I didn’t need to look at it at that moment, eventually I would have to look at my leg. I had shorts on (as requested) so it was hard not to see the 7 inch scar that now divided the center of my leg into halves. Tears started flowing because that seems to be what I do now when I see physical therapists. Ingrid asked me if it hurt. Not physically, I answered, but it no longer looked like my leg. I’m not familiar with my new leg and for some reason it’s making me sad. She nodded and gave me the box of Kleenex from a nearby table and we proceeded with the exercises. In between exercises she stopped, looked at me and said,
“It’s probably a good thing you didn’t go into the medical field… you know, with the whole bleeding thing and all…”
Ingrid is serious and focused, and doesn’t say much, but what she does say makes me smile.
“Yea, I’d have my eyes closed too much to be good in the medical field,” I confirmed.
I couldn’t help but think about what a friend had told me regarding her first PT appointment and how she sobbed the entire time, not really knowing why. Maybe her telling me that had freed me up for doing the same. It’s sure easier than holding back the tears. Another friend who had gone through a knee replacement a few months earlier told me not forget the emotional aspect of a knee replacement, even though the physical part is the part that gets all the attention. I didn’t really understand what she meant when she told me that just days after my surgery, but I do now as I’m trying to find ease and comfort with something that isn’t either. Ingrid told me that as much as I’m getting used to the new knee, the new knee is also getting used to me. And that’s when I named her. If I’m going to have this part of my body tag along with me for the rest of my life, the least I can do is try to become more familiar with her and giving her a name felt like a good start. Her name is Rhoda. It came to me instantly, but there could be a lot of reasons for her name. First off, the character in the Mary Tyler Moore show, who was my favorite — the outspoken, bohemian, free-spirited woman who lived upstairs — the character who I felt I had a better chance being like than Mary, the star of the show. And secondly, rodilla is knee in Spanish, and I always love giving the language I’ve spent so much time trying to learn some recognition. And so I named her Rhoda.
Before I left the physical therapist office, my therapist’s assistant, Esther, said something about a client she had come in right before me and I thought she said her name was Samantha. When I asked what body part Samantha was working on, Esther quickly corrected me and said,
“Oh that’s not the patient’s name. It’s her new shoulder’s name.”
I’m right in line with Rhoda. Given that I see my physical therapists twice a week for at least a few months, I need to make sure they are both properly introduced to Rhoda. They may also offer her apologies in advance for the pain they might inflict during future appointments.
And so my journey continues… days are slow, weeks are faster. I’d much rather be writing about walking adventures in other countries and my discoveries encountered along the way, but instead, I’ll continue to record the journey of the hinge in the center of my left leg that is forging its own trails as it learns to bend. It’s not as exciting as the walks I’ve written about for so many of the past Septembers and Octobers, but trust me, it’s every bit as hard as an 18 miles day climbing uphill, with a head wind in the Pyrenees. Just not as scenic.
